When I first discussed going on hormones with my psychotherapist he asked if I was thinking of going public or private. “I’ve heard about Loughlinstown”, was my response.“ So, private then”, they concluded. I nodded with a sigh.
I will be looking here at the path to hormones, as that is a common desire for trans people including myself. However, it is not required to be on, or even want, hormones to be trans. There are many trans experiences. One person might only desire surgery while another may be satisfied with changing their pronouns.
For adults needing to look for hormones within the framework of public transgender healthcare, Ireland’s only provider is the National Gender Service (NGS) hosted in St. Columcille’s Hospital, Loughlinstown. It is commonly referred to as just Loughlinstown. Most of what I personally know of it is second hand; from ever-longer waiting lists, invasive questions, and the odd report of a good experience. It’d be nice to have reliable information. So I went looking to see what I could find.
Information wants to be free
In the past month Loughlinstown launched a website which has information on the service, including “We are currently seeing people referred two and a half years ago”. The attentive reader will notice that this is not the same as saying that someone referred today will be seen in two and a half years. For example, one of the Gender Identity Clinics (GIC) in the UK is seeing referrals from four years ago, while a new patient could be waiting nineteen years.
So what do things look like here in Ireland?
To help add hard data to the situation I sent in a Freedom of Information (FoI) request to the Dublin Mid-Leinster hospital group which Loughlinstown is a part of. I asked questions around the size of the waiting list, and how quickly people are being added, removed, and assessed. I asked for both 2019 and 2020 data, as 2020 data alone is unlikely to be representative given that COVID presumably caused some level of service disruption.
I got my response two weeks later with the following key points:
As of August 2021, there are 790 people waiting.
At the end of 2020 there were 664 people waiting.
268 people added in 2019 are still waiting.
321 people were added in 2020.

Unfortunately much of my request was not granted. However the response included informative context as to why. For example, a specific waiting list for the National Gender Service didn’t exist in 2019, and gathering details on assessment/removal would require manually digging through patient charts. They do however hope that, funding permitting, in 2022 there will be an appropriate IT system which can extract such data.
Hurry up and wait
While on the surface it may look like there’s not enough information in the FoI response to calculate the length of the wait, with a bit of math you could get a good idea. Another approach would be to use other publicly available information, for example the fact that 420 people are being referred, and up to 150 people can be seen a year.
There’s still a third of the year to go from August so another 140 will be referred and 50 seen. So the list is expected to go from 790 in August to 980 people at the end of 2021. With at most 150 people seen in a year, someone referred at the end of 2021 would be waiting over six and a half years to be scheduled for initial assessment.
That initial assessment is expected to take four to five hours across two visits, after which you may get an endocrine appointment to discuss hormones. The FoI revealed that 35% people will need more than two visits for initial assessment.
Forward-looking statements
For someone referred to Loughlinstown this year the wait is over 6 years. What about someone referred in 2022?
I’ve combined a variety of sources for statistics including scientific papers, newspaper articles and the service model proposal to show the growth in referrals over time.
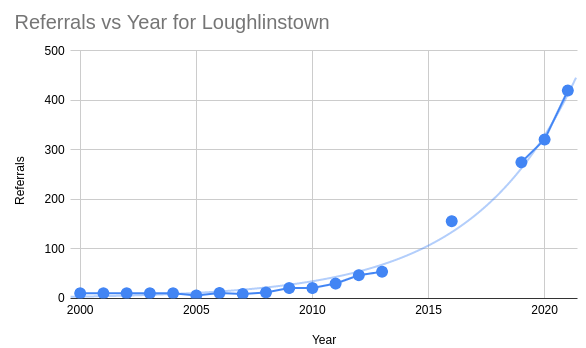
The curve is exponential, showing a 30% growth in referrals every year. So 546 people are expected to be referred in 2022, bringing the waiting list to 1376 people by the end of that year for a nine-year wait. I’ve graphed how this would look over the coming years if 150 people continue to be seen every year.

If the trend continues, by the end of the decade a new referral would be expected to wait over 80 years due to the 12,000 people already on the waiting list. Given that trans people are estimated at 1-2% of the population, this is unfortunately well within the realms of possibility. If anything it might be an underestimate.
A better approach
The current model of public trans healthcare is nowhere near sufficient for the current level of need, let alone expected growth. I am privileged enough to be able to avail of private services like GenderGP. But I know many others who have to wait in hope that the public healthcare system will provide for them many years down the line.
We need something more fit for purpose than specialised centres that require a minimum of four or five hours of assessment per person. Why not follow other countries and allow GPs to handle basic trans healthcare on an informed consent model? Why not let the specialist consultants focus on more complex cases better suited to their talents?
For the majority of trans people, hormones are quite simple to manage from a medical standpoint. GPs already commonly prescribe Hormone Replacement Therapy (HRT) for postmenopause, and these are in fact some of the exact medicines used in trans healthcare. Monitoring hormones for HRT is no more difficult than monitoring conditions such as diabetes which is regularly managed by GPs as it is.
Irish hospitals are already overstretched. So why put more resources into an archaic overcomplicated system that’s not fit for purpose when people can and should be handled by their GP instead?
At the end of the day, we want the same thing everyone else wants and is entitled to: Prompt, effective, and efficient healthcare in line with international best practice so that we can continue with our lives in peace.
Jessica Black (she/her) is an Irish lady who dabbles in statistics from time to time.
Featured image via Facebook – GCN
